Dominique Vervoort and Ge Bai analyzed the percentage change in average charges and compared them to average Medicare Part B (fee-for-service) payments for 51 specialties. Data was drawn from the years 2010 to 2019, with the figures adjusted for inflation.
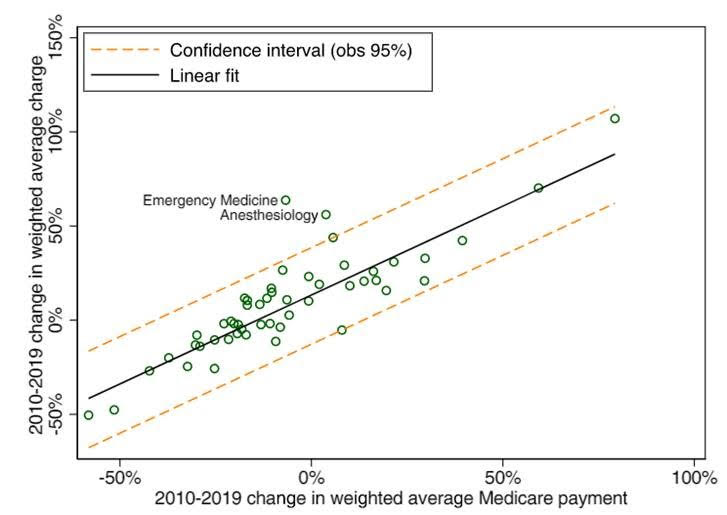
The authors found a positive association between the change in charges and change in Medicare payments (see the figure). This was not unexpected. Charges are often pegged to Medicare in some way. There were two outliers. (This too should come as no surprise). Emergency care and anesthesia charges grew faster and were above the trend line. According to the authors:
[T]he identification of emergency medicine and anesthesiology as outlier medical specialties with disproportionately high growth in charges contributes to the literature on surprise out-of-network balance billing. Although patients may have some options in choosing where to receive emergency care or surgery, they often cannot exercise options in selecting emergency physicians or anesthesiologists.
What emergency medicine and anesthesia both have in common is patients rarely have the opportunity to select their providers, or even meet them prior to care. As a result, these providers often refuse to join networks, allowing them to charge higher fees and balance-bill patients for the portion health plans do not pay. The authors say it remains to be seen whether the No Surprises Act of 2020 will mitigate balance-billing.
Source: Dominique Vervoort and Ge Bai, “The Identification of Outlier Medical Specialties from Examining the Association Between the Change in Charges and the Change in Medicare Payments from 2010 to 2019,” Journal of General Internal Medicine, March 14, 2022.

I would love to hear y’alls take on this latest surprise bill for an emergency flight.
https://www.npr.org/sections/health-shots/2022/03/25/1088663449/the-case-of-the-489-000-air-ambulance-ride
If you look closely at the scatterplot, just below anesthesiology is a small circle that is on the verge of being an outlier. I looked at the data and that is critical care. What do all these have in common? You are not in a position to negotiate, bargain or walk away if you need the services of an emergency physician, anesthesiologist or a critical care physician.