During the initial outbreaks of Covid there was a shortage of ventilators, used to help patients breathe:
A ventilator is a piece of medical technology that provides mechanical ventilation by moving breathable air into and out of the lungs, to deliver breaths to a patient who is physically unable to breathe, or breathing insufficiently. Ventilators are computerized microprocessor-controlled machines, but patients can also be ventilated with a simple, hand-operated bag valve mask.
Not long after Covid took hold in 2020 the price of ventilators shot up from about $25,00 to $50,000 apiece due to increased demand. Some researchers attempted to make ventilators out of scavenged parts and items from hardware stores. A team at MIT designed one that cost about $100 to build. It was made using a bag-valve resuscitator, an item commonly found in hospitals. So too did a University of Florida professor:
Lampotang dispatched David Lizdas, Ph.D., the lead engineer in his lab, to Home Depot to gather items such as air-tight PVC water pipes and lawn-sprinkler valves. Along with engineering and medical colleagues at UF and — through a burgeoning open-source network — places as far-flung as Canada, India, Ireland, Vietnam and Brazil, they raced to “MacGyver” these items and other pieces, including a microcontroller board and a ham radio DC power supply, into an open-source ventilator…
As did researchers from Vanderbilt University:
Webster is working with other engineers… building this out of regular household stuff in their garage rather than out of their usual fancy equipment.
“Pieces of wood, plywood. This is a car windshield wiper motor,” he said as he showed off the current design.
They’re also using regular door glides.
These doctors, professors, mechanical engineers and other experts worked to replicate quickly and cheaply what had already been invented nearly 70 years earlier. It’s a fascinating story that was covered by Smithsonian magazine and recently reprinted in GetPocket.
Seven decades before COVID-19, a similar crisis strained the city of Copenhagen. In August 1952, the Blegdam Hospital was unprepared and overwhelmed. A 12-year-old victim, Vivi Ebert, lay paralyzed before anesthesiologist Bjørn Ibsen, “gasping for air” and “drowning in her own secretions.”
With his hands, a rubber bag, and a curved metal tube, Ibsen reset the boundary between life and death and taught the world how to breathe.
The Polio virus was the plague that attacked Copenhagen in the Summer of 1952. The outbreak was the worst of any city in Europe and the U.S. Many victims died when they could no longer breathe.
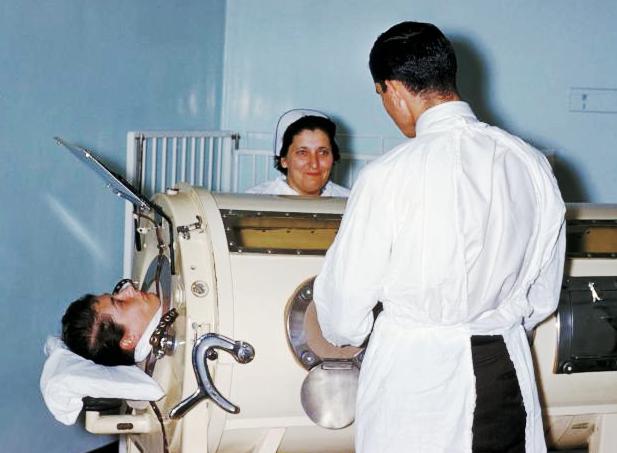
Waves of young people with fever, headache, upset stomach and stiff neck heralded the arrival of the “summer plague” in cities throughout the United States and Europe. Masquerading as a common stomach virus, the infection established itself in the gut before spreading to the brain and spinal cord. The clinical picture ranged from a self-limited stomach bug to paralysis, shock and asphyxia. Some recovered, but lasting disability, or death, was typical. At the time, the best way to treat respiratory complications of polio was with the “iron lung,” a tank that encased polio victims but allowed them to breathe with the help of a vacuum pump.
In addition to iron lungs, later there was a rocking table bed with an axle in the middle. By rocking the table moved the chest up and down causing shallow breathing as the patients guts pushed and released against their diaphragm.
Ibsen… suspected that paralyzed chest muscles compromised respiration. The lungs themselves could sustain life if stronger mechanical muscles could be found. A world war and a chance encounter would lead him to the solution—and to an ethical dilemma that spurred accusations of murder.
In Boston [1950], Ibsen learned the art of “bagging”—the use of a hand-squeezed rubber bag to breathe for anesthetized patients during surgery; the practice was foreign to Danish physicians at the time.
Ibsen’s bagging, known as “positive pressure ventilation,” was not widely used at the time, as it contradicted human physiology. Normally, air is instead drawn into the lungs by negative pressure—the vacuum created by diaphragm and chest muscle contraction. Outside of the operating room, negative pressure ventilators, such as Blegdam’s “iron lung,” were the sole means of artificial respiration.
Using a barbiturate to calm her choking reflex, Ibsen was able to use a bag to inflate Vivi Ebert’s lungs. She improved but deteriorated again when manual ventilation stopped. It seemed possible that she – and others – could live if they had a way to continue squeezing the bag. Volunteers were recruited to bag respirate up to 70 polio patients around the clock.
Few medical innovations would be so immediate and definitive. In one week, the mortality of bulbar polio fell from 87 to barely 50 percent. By November, the death rate dropped again to 36 percent. As the embers of the Copenhagen outbreak cooled in March 1953, only 11 percent of patients who developed bulbar polio died.
The problem with iron lungs, rocking tables and mechanical ventilators: what if care has to be permanent? What if patients can survive on the ventilator but not without the technology? That created an ethical dilemma.
What happens if the patient cannot be weaned from the ventilator? What happens when the body recovers and the mind does not? Does life support benefit all patients? Should intensive care be offered to everyone? The ethical and social weight of these concerns saddled Ibsen with somewhat conflicting roles as proud father and emerging conscience of this new brand of medicine.
Indeed, that is exactly what happened.
In October 1953, well past the one-year anniversary of Vivi Ebert’s rescue, 20 of the original 318 patients treated by Ibsen’s method still required around-the-clock ventilation at Blegdam Hospital. By 1956, 13 patients remained dependent.
Ibsen’s original patient, Vivi Elbert, required continuous ventilate from August 1952 to January 1953. But that wasn’t the end of it:
Quadriplegic, but alive, she left Blegdam in 1959 after a seven-year convalescence. After discharge, she moved with her mother, Karen, and a devoted rough collie named Bobby to an apartment complex for polio survivors. She relied on Karen for most daily needs like eating and toileting. Every evening, Vivi was wheeled to a penthouse unit where she slept on a ventilator under medical supervision.
Vivi Elbert completed her education from a wheelchair. She could turn pages of a book and even type with a stick held in her mouth. She got married but later separated from her husband. She died of pneumonia and sepsis in 1971 at age 31.
When asked if ventilators sometimes just prolonged the inevitable, Ibsen admitted it was often true. He also admitted to disconnecting patients from ventilators who had no chance of surviving. His admission created a firestorm of controversy. He lost his hospital privilages but faced no legal action.
How could you write this post without addressing the charge that ventilators were inappropriate for covid patients and created many of the early deaths. British research first suggested this might be the case.